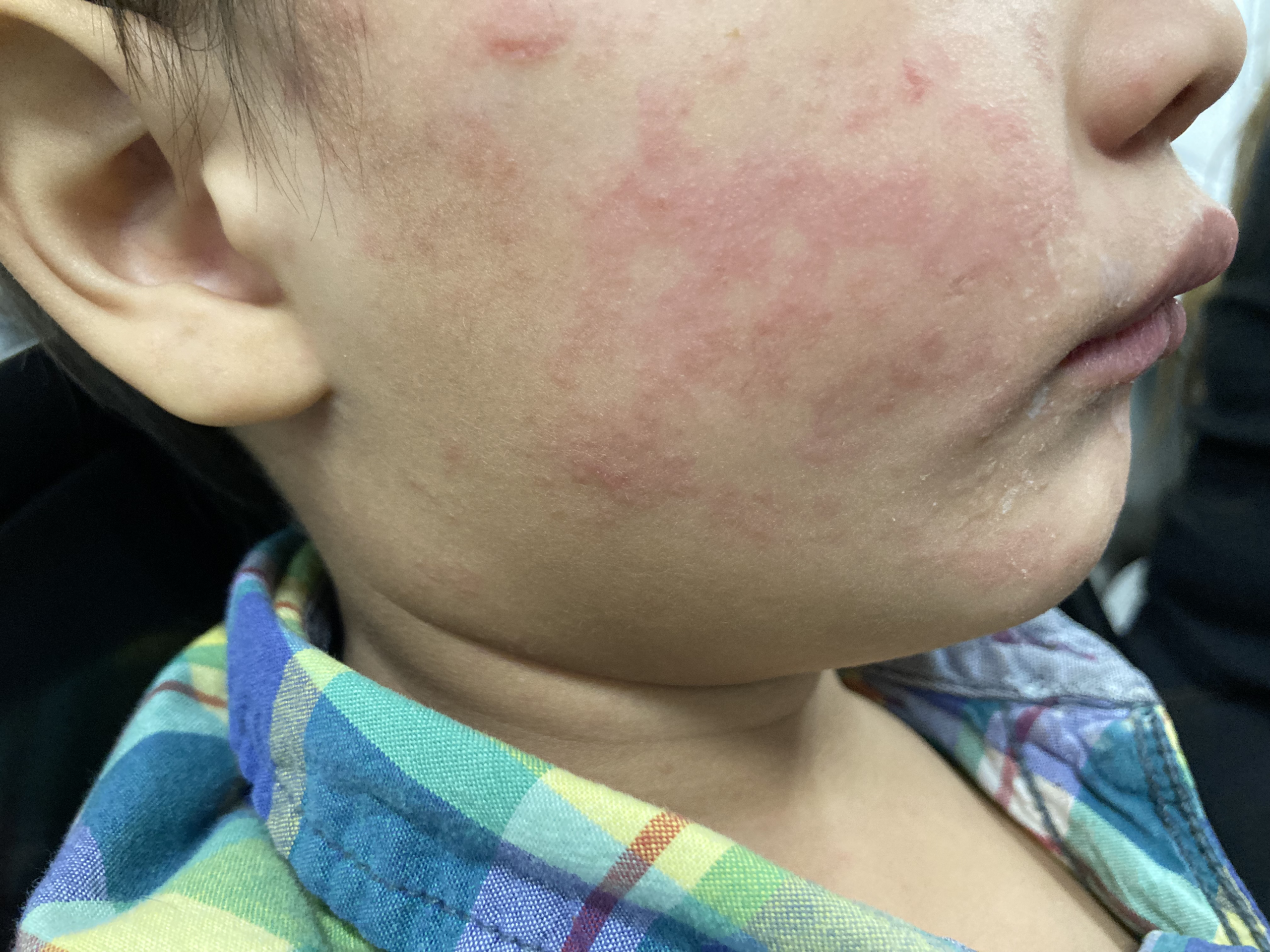
Measles 2025: A Retrospective on a Record-Breaking Year
2025 was the worst year for measles in the US since 1992.
According to the US Centers for Disease Control and Prevention (CDC), at the close of 2025 there were more than 2,250 confirmed cases of measles in the country. Compare that to 285 in 2024 and 59 in 2023.
And that’s just what was reported.
Officials suspect many more cases circulated around the country but because some patients did not seek medical care, they weren’t part of the official count. In Texas, for example, where there were 762 confirmed cases last year, experts estimate another 200-300 people were infected but not counted.
Measles is a viral infection characterized by a rash, fever, cough and runny nose. It’s particularly dangerous in children younger than five and is so contagious, CDC reports that nine out of 10 unprotected people will become infected with the virus if they are in contact with someone who has it. Three people died from measles in 2025.
On the precipice
In 2000, measles was officially eliminated in the US. A disease is considered eliminated when it is no longer spreading within the country.
But 49 measles outbreaks (defined as three or more related cases) were reported around the country last year, stretching from Alabama to Alaska, Vermont to Virginia, South Carolina to South Dakota. And 89% of 2025’s measles cases were associated with outbreaks.
These numbers indicate that measles is on the rise within the country, putting the US at serious risk of losing its elimination status—something that recently occurred in Canada.
What’s needed to prevent more cases? Public health professionals point to increased detection, more timely outbreak response and the use of medical interventions that can prevent viruses from taking hold.
Playing a key role are the public health laboratories that identify and track diseases like measles. Their testing gives clinicians the crucial information they need to make appropriate diagnoses so patients can receive the kind of prompt treatment that saves lives and curtails outbreaks. Their testing also contributes to understanding measles transmission, a requirement to understanding the linkage between different outbreaks or new introductions of the virus.
How have some states and their public health laboratories responded to measles outbreaks in the last year? We take a look back.
Texas
Texas had the unwelcome distinction of being home to the largest measles outbreak in the country last year. There were 762 confirmed cases reported between January and August (when the outbreak was declared over), with most of those cases located in the western portion of the state where close-knit communities with low vaccination rates live.
And the first case that started it all had public health officials puzzled.
The patient reported no recent travel, meaning the infection had to come from within the community. What’s more, genotyping identified the strain as D8, a strain recently seen in Canada and Mexico, but—at least at the time—not often seen in the US.
“We don’t know how this person picked up this strain,” said Grace Kubin, PhD, deputy commissioner/laboratory director, Public Health Laboratory Division, Texas Department of State Health Services. “But members of the community that this person belongs to travel back and forth between Mexico and Canada, where they tend to have family and friends. We’re trying to work with Canada to do sequencing related to this strain to see if there’s a link.”
Given the contagiousness of measles, it’s no surprise that cases began exploding. But luckily, said Kubin, because of previous measles outbreaks in the state, Texas was prepared to handle the influx of testing.
“We had PCR tests, which are rapid tests that can detect active infections,” Kubin explained. One problem, though: The PCR throughput was low, allowing for the processing of only about 22 samples per PCR run.
“When the outbreak really started spiraling, we had two PCR machines validated for the measles test,” Kubin noted, “and we had staff who had to manually extract the nucleic acid. We had to switch gears and work on automated extraction methods and validate two more PCR machines for measles testing to keep up with the volume.” The lab also acquired a high throughput instrument, which could process 800 tests a day “pretty easily,” said Kubin.
By early spring, the Texas state public health laboratory as well as CDC-supported Laboratory Response Network (LRN) labs across the state were handling a large volume of measles tests. (LRN laboratories respond to biological and chemical threats as well as other public health emergencies.) Samples originally were being sent to Minnesota, one of four APHL/CDC Vaccine Preventable Disease (VPD) Reference Centers, for genotyping but by April, Kubin said, labs in Texas were able to take the job over.
“I think we had a couple of cases that were related to international travel, so they weren’t classified as part of this outbreak,” Kubin stated, “but almost all the other samples were D8 strains. We’re also comparing our samples to the outbreak in Utah, and those strains are also D8.” Despite being the same strain, Kubin noted that when the phylogenetic trees (the evolutionary history between a set of species) are examined, the samples are different, indicating that the Utah outbreak is unrelated to the one in Texas.
The Texas outbreak was declared over in mid-August, thanks to increased health messaging, pop-up vaccine clinics and webinars educating health care workers—many of whom had never seen a measles rash in person—on the signs and symptoms of the infection.
“This was a collaborative and massive response, and I really can’t give enough kudos to the local public health officials in the hot spot areas,” Kubin said. “Responding to this outbreak is a perfect example of what public health laboratories do—we perform tests that may not be available to other labs, and we will keep performing these tests as long as it’s vital to public health action.”
Utah
There have been more than 200 confirmed measles cases in Utah since its current outbreak began last year. And 55 of those cases were diagnosed in the last few weeks alone.
When the state’s outbreak started last summer, the Utah Public Health Laboratory (UPHL) didn’t have a nucleic acid PCR test available, said Alessandro Rossi, PhD, CLIA director and infectious diseases chief scientist at UPHL. Until the state’s testing could be ramped up, specimens from patients suspected of having measles were sent to the VPD Reference Center in California, commercial labs and the Arizona State Public Health Laboratory.
“Eventually, we were able to validate a multiplex PCR test on Panther Fusion, which is based on two tests developed by CDC and other public health groups,” Rossi said. “The test can detect both wild type [naturally occurring, nonvaccine viral strains] and the vaccine strain.”
To understand where the virus was spreading—often before patients even noticed symptoms—UPHL started wastewater surveillance later in the summer. Currently, it monitors 35 community wastewater systems across Utah, covering approximately 85% of the state’s population.
“Utah has regions with notably low vaccination coverage, increasing the risk of community spread,” said German Pinas, PhD, manager of Water Microbiology and Wastewater Surveillance at the Utah Public Health Laboratory. “Additionally, our somewhat geographic proximity to Texas—where the first major outbreak occurred—added urgency and reinforced the value of an early, population-level detection system.”
Pinas explained that the wastewater surveillance uses the highly sensitive droplet-digital PCR test to quantify the measles viral load in a wastewater sample. “We also perform sequencing for viral strain and sub-strain identification, which helps determine if cases are related to the current outbreak,” he noted. “While the initial epicenter of the outbreak was in southwest Utah, we’re now detecting cases emerging in northern and central regions as well. The statewide coverage allows us to track spread beyond the original hotspot.”
South Carolina
South Carolina is still in the midst of its measles outbreak, which began last October. Since the first person was diagnosed, cases have exploded. As of late January, there have been 789 cases—and counting. Nearly 100 were reported in just three days in early January.
The outbreak is centered in Spartanburg County, in the state’s northwest region. While some of the cases seem to have spread via travel or were acquired from the close contact of a known case, others have no known source, indicating the virus—whether diagnosed or not—is circulating in the community.
In response to the outbreak, the public health laboratory in South Carolina has cross-trained additional staff to ensure adequate testing capacity.
“The virology unit, which is responsible for outbreak-related viral testing, has always practiced broad cross-training to maximize response capacity,” said Cory Weaver, PhD, South Carolina Public Health Laboratory (SC PHL) section director – Virology, Serology & Advanced Molecular. “All team members are trained to perform critical testing for outbreak responses. During the outbreak, virology staff have worked extensively with clinicians and state epidemiologists to provide specimen collection supplies and advise proper collection methods. The lab has developed simple, single-page guidance documents to assist field epidemiology staff in specimen collection.”
Leaning on the expertise of both state and federal partners has also been key, Weaver noted. For example, samples have been sent to CDC and Wadsworth Center (which serves as South Carolina’s VPD Reference Center) for genotyping using Sanger sequencing.
“While genotyping does not allow for tracing the source and transmission routes of the virus for specific cases,” Weaver added, “it does provide important information about the specific strain circulating in South Carolina.”
Public health officials in the state have also called on the skills of their counterparts in Colorado and Utah. The SC PHL is collaborating with the UPHL to perform whole genome sequencing (WGS) on clinical samples while South Carolina builds its in-house sequencing capacity. According to Weaver, WGS will provide deeper insights into strain circulation patterns and contribute to improved national measles surveillance.
The SC PHL is also working with the Colorado Laboratory Services Division, a National Wastewater Surveillance System Center of Excellence, for wastewater monitoring. The Colorado PHL provided technical assistance as South Carolina implemented routine measles wastewater surveillance. Now, South Carolina is sending positive wastewater samples to Colorado for genotyping and WGS.
“The support from CDC and our colleagues across the country has been invaluable to our response,” Weaver said.
Despite its efforts, South Carolina’s measles outbreak is far from over. Public health officials predict the outbreak will last into the spring—at least.
“We expect many more cases in the area because of low vaccination coverage,” said State Epidemiologist Linda Bell, MD. “The department is working to contain the outbreak to its current center of Spartanburg County and prevent the spread to other parts of South Carolina and other states. Measles is highly infectious and spread elsewhere is possible because vaccination coverage in some areas isn’t high enough for herd immunity.”
Even as South Carolina battles its current outbreak, it prepares for future ones by building automated, high-throughput methods for measles RT-PCR testing and expanding in-house viral sequencing capability with a focus on rapid response to new pathogens. “This will provide more timely, robust genomic data for future outbreaks,” Weaver said.
The importance of adequate funding
PHLs—like those highlighted here—receive crucial funding through CDC’s Epidemiology and Laboratory Capacity for Prevention and Control of Emerging Infectious Diseases (ELC) Cooperative Agreement. ELC funding strengthens the ability of PHLs to rapidly detect and respond to disease outbreaks, including these measles outbreaks.
It’s funding that gives these laboratories the ability to secure the additional testing supplies and instrumentation needed to handle the influx of specimens an outbreak brings. It also gives them the financial ability to properly maintain that instrumentation, train staff on its usage (and hire additional personnel if needed), contract with courier services and keep data reporting systems up to date through flexible cross-cutting funding lines. All of this adds up to faster diagnosis, faster treatment and a faster end to an outbreak.
And as important as detection is, so is response.
In addition to securing supplies and ensuring a properly trained workforce, ELC funding enables public health professionals to devise and disseminate important public health messaging while also performing community outreach, informing people about how the disease is spread and how it can be prevented. When funding is cut—or worse yet, lost—disease detection takes longer, outbreaks grow and lives that otherwise could have been saved are lost.